Cart is empty
Home/Our Publications/Educational Articles/Potential Causes of Nosocomial Type Infections in the Salon-Clinic Setting
Potential Causes of Nosocomial Type Infections in the Salon-Clinic Setting
24/04/2013
by Andrea Darby - Master Medical Tattooist & Industry Educator
Important: This article is a general discussion paper regarding some of the potential causes of Salon Acquired Infections and is not intended to be an exhaustive explanation or review of all matters relating to infection prevention. This publication does not suggest that SAI are the commonest cause of post tattoo infections or the cause of an infection in any particular case. Any matters raised are purely for discussion and do not represent the regulatory position in any geographical domain.
▼ Continue Reading ▼
|
Introduction The term “nosocomial” originates from the Greek words “nosus” (disease) and “komeion” (to take care of). Therefore by strict definition “nosocomial” means an infectious disease that is contracted by a person whilst under the care of others.
There is an absence of wide scale reliable data in relation to the incidence nosocomial type infections acquired in Cosmetic Tattoo Salon-Clinic settings, to avoid confusion we will refer to that type of occurrence as a Salon Acquired Infection (SAI). A review of the medical literature did however reveal some studies and reports with broader relevance to the beauty and tattoo industry.
A Brazilian study by Department of Epidemiology and Biostatistics, McGill University, Montreal, Canada concluded that having a tattoo is not an important indicator for testing positive for transfusion-transmitted diseases (blood borne communicable diseases), except for HCV infection3.
The differences between those studies may be in part due to the fact that the Amsterdam study accounted for the prevalence of infections in the countries in which the individual obtained their tattoos for those who underwent tattooing outside of the Netherlands. Also there may be significant regulatory differences in different geographical locations and from a statistical perspective small scale studies may be less reliable.
A large study (n642) conducted by the Centre for Epidemiology and Population Health Research, Macfarlane Burnet Institute for Medical Research and Public Health in Victoria Australia4 found that HCV antibody-positive prisoners were more likely to have acquired a tattoo in prison compared with HCV antibody-negative prisoners. The study also found that of those who did not receive their tattooing from a professional tattooist 27% of them indicated that the same needle had been used on another person. Richard Griffith from the College of Human and Health Sciences, Swansea University United Kingdom argues that; the public health risk to children from the use of un-sterile home tattooing equipment is so great that a repeal of the Tattooing of Minors Act 1969 within that country may be warranted, presumably to ensure that juveniles who undergo tattooing will at least have access to qualified tattooists providing services under hygienic conditions34.
Undoubtedly the greatest risk of transmission of a BBCD via tattooing is if tattoo services are provided without strict adherence to standard precautions and general hygiene recommendations and that situation is most likely to occur if tattoos are obtained from a person who is not a professionally trained tattooist.
We also discovered a case report from China of secondary syphilis presenting in a tattoo5, it is believed that the unhygienic practice of diluting pigment with the saliva of the tattooist was the causal factor in that particular case. This highlights the potential risk of undergoing tattooing whilst travelling overseas unless there is a high degree of confidence in the hygiene practices and regulatory oversight of the tattoo industry within the country being visited.
Another study conducted in La Rioja Spain found that of 138 women who received mesotherapy (skin needling) at a single beauty salon 28.3% (n39/138) developed lesions thought to be caused by mycobacterium fortuitum infection6, underscoring the potential risks associated with dermal rollers and similar apparatus.
There are numerous case reports within the medical literature of outbreaks of infections with various forms of mycobacterium at nail salons providing manicure and pedicures7, 8, 9, 10, 11, 12, 13. Perhaps the most pertinent aspect relating to the Cosmetic Tattoo industry is the increased potential for Salon Acquired Infections if other services that have higher incidences of infections such as manicures / pedicures are conducted at the same location as the cosmetic tattoo service.
In addition to the reports that directly relate to Salon Acquired Infections our colleagues working in various professional health service settings have conducted a wide range of studies that we can utilise to evaluate some of the areas that may present an increased risk of SAI and we can adapt our procedures accordingly.
Industry Background Cosmetic tattooists come from a diverse range of educational backgrounds; some are also qualified health professionals such as nurses, doctors, and dermal clinicians, overwhelmingly most Cosmetic Tattooists appear to have come from backgrounds in the beauty industry.
From our own experience most cosmetic tattooist do appear to be aware that services should be delivered using “standard precautions” and in particular the need for single use sterile needles to help prevent the transmission of blood borne communicable disease. However we often see the term “aseptic technique” being misused to describe procedural methods that would be better described simply as “clean technique” and there does not always appear to be a high level of recognition of the potential for the broader range of nosocomial type Salon Acquired Infections that may occur.
Procedural Techniques “Aseptic Technique” is a clearly defined procedural approach used by health professionals in a clinical or hospital setting to prevent the contamination of wounds and other sites such as intravenous cannulas, urinary catheters, central venous lines etc by micro-organisms. Aseptic technique is also used to help prevent cross contamination/infections between patients, staff, equipment and environmental surfaces.
In most countries among the various groups of health professionals there is a relatively high degree of uniformity in application of the underlying principles of aseptic technique and a clear recognition of the differences between the following standards;
Our observation is that within the salon environment and procedures used for Cosmetic Tattooing the standards often fall somewhere between Clean/Hygienic Technique and Clinical/Medical Asepsis with a bias towards the former. Ideally Cosmetic Tattoo procedures would be performed utilising defined aseptic techniques as the required standard (Grade 2 Asepsis) and medical tattoo procedures conducted within an operating room would of course be conducted at Surgical Asepsis standard (Grade 1 Asepsis).
Regardless of the geographical location most qualified health care providers are aware of the need for and differentiation of levels of asepsis with procedural doctrines, likely this is due to “aseptic technique” forming part of most base education programs for most health professionals. However we have observed that there is often confusion about this topic within the Cosmetic Tattoo industry.
In addition to misunderstandings about what is required with “aseptic technique” (Grade 2 Asepsis) we have often encountered misconceptions about the distinction between;
Even some of the best hospital facilities have developed serious public health problems due to a small break down in their asepsis procedures.
Regulatory Requirements for Cosmetic Tattooists There are numerous differences in regulatory requirements in different geographical domains, understandably most of the regulations that we have examined appear to be primarily focused on the prevention of transmission of Blood Borne Communicable Disease (BBCD). There is also often a focus upon the prevention of wound infections via the mention of Grade 3 Asepsis type requirements.
Discussion In most locations there seems to be a high level of general awareness of the need for procedures that prevent the transmission of BBCD’s, health authorities such as the World Health Organisation have done an exceptional job of informing and educating via their health publications such as “Standard precautions in health care”.
We will therefore focus on a broader range of potential risks that may result in a Salon Acquired Infection (SAI) and will draw from the medical literature to highlight some of the less obvious causes.
Potential Causes of Salon Acquired Infections There are 5 primary areas of concern;
Factors inherent to the Client / Patient At any given time each of us has literally billions of micro-organisms living on our bodies, on our skin, hair, nails, conjunctiva, respiratory system, digestive system and literally inside our cells. It has been estimated that our digestive system alone may have up to 100014 different species of bacteria residing in it.
Some of the micro-organisms that live on and within our bodies provide a useful service such as aiding digestion within our gut, many of the micro-organisms we simply do not know enough about to know if they are helpful to us or not. Some micro-organisms are pathogenic (disease causing) having the potential to cause minor and sometimes major illness.
We have an intimate relationship with micro-organisms and our good health depends upon our mutually beneficial arrangement with these tiny creatures, those residing on us are often referred to as our natural flora or the human microbiota. Studies conducted by environmental scientists15 showed that within an indoor space around 18% of the microbes within the air came from the humans within the room and that the average person sheds up to 37,000,000 bacteria into the air every hour.
The mere presence of a person in a room adds millions of micro-organisms to the environment without them ever physically touching any object within the room due to the constant emission of our own microbiotal plume.
Significantly the same study also found that 15% of those within the case group had Diabetes Mellitus compared to 7% in the control group and 36% of those in the case group had a skin infection in the previous 6 months compared to just 1% of the control group. Even among the extended members of the household 26% of those within the case group had a person in the household who had experienced a skin infection within the previous 6 months compared to just 7% in the control group. Some hospitals have begun routinely swabbing patients for the existence of antibiotic resistant pathogens prior to performing surgical procedures, ABC's Catalyst dives into this topic in the video below.
Once the skin surface is broken by a Cosmetic Tattoo procedure any micro-organisms that may be residing on the surface of the skin or in the client/patients home and working environment have the potential to gain entry via the open wound and cause a post procedure infection. Whilst strictly speaking this type of infection would not be regarded as a Salon Acquired Infection the act of piercing the skin provides a potential portal of entry for pathogenic organisms and therefore preventative aftercare advice is an essential part of any cosmetic tattoo procedure.
A well known lanolin based antiseptic nappy care cream has probably been the most commonly used tattoo aftercare cream by both cosmetic tattooists and the body art industry. There are a range of purpose specific alternatives in the market place which may claim superior results or reduced healing times. In 2012 researchers from the university of Worcester United Kingdom published a study evaluating the efficacy of a purpose designed tattoo after care cream in comparison to the commonly used nappy care cream17 the results of the study found no statistical differences between the purpose-designed post-tattoo cream and the nappy care cream.
The Worchester study is particularly significant as it claims to be the first randomised, controlled, double blind clinical trial that has been conducted to evaluate skin function relative to topical preparations in treatment of tattoo aftercare. Useful information from the study includes; 1) Oedema (swelling) was found to have the greatest improvement between day 0-4 post tattooing with no swelling evident by day 14. 2) Mean skin hydration values and transepidermal water loss (TEWL) both showed significant improvement by day 7 post tattooing and a further steady improvement in both values up to day 28.
The Worchester study highlights the critical role aftercare plays in both infection prevention and supporting skin hydration during the 28 days post tattooing and particularly the initial 7 days.
Key Points:
Factors Relating to the Cosmetic Tattooist & Other Staff Those engaged in skin penetration procedures should have clearly defined written guidelines for client/patient treatments and for cleaning, disinfection and waste disposal. The most likely way that a Cosmetic Tattooist and other Salon staff may have the potential to contribute to Salon Acquired Infections is due to the use of inadequate aseptic techniques or a failure to comply with asepsis/hygiene procedures.
Even among well educated health professionals there can be potential problems arising from basic hygiene standards and personal attire. The infectious Disease Unit, Shaare Zedek Medical Center, Hebrew University-Hadassah Medical School, Jerusalem, Israel conducted a study to asses if the clothing/uniforms of doctors and nurses could be a potential source of nosocomial infections18.
In 2012 a small scale study was published by Cornell University in lthaca, NY, USA examining if women doctors' purses could be a previously unrecognized fomite19. The results of the study found that 69% (n9/13) of the swabbed doctors purses were colonized with bacteria compared with just 14% (n2/14) in the control group. This study highlights the importance of adequate hand washing procedures and the appropriate use of examination gloves as well as the potential for any object in the salon-clinic environment to be a fomite.
It would be prudent for Cosmetic Tattooists and other salon-clinic staff to routinely revisit their personal hygiene and aseptic techniques to ensure that their practices do not become the weak point in the overall standard of asepsis provided to clients/patients.
Key Points:
Procedural Equipment & Supplies The hands of staff and procedural equipment and supplies have the highest risk of direct contamination of the client/patients skin during a cosmetic tattoo procedure.
Some Cosmetic Tattooists appear to have a dilemma when making choices about the grade of equipment and procedural supplies to utilise for client/patient services. The decision however is relatively straight forward, wherever possible supplies should be sourced from reputable manufacturers and suppliers and be sterile Clinical/Medical grade. Sterile supplies should detail the sterilization method and the expiry date and if requested the manufacturer should be able to provide a certificate of sterilization.
Special attention should be paid to re-usable equipment and supplies to ensure that they do not become contaminated and result in cross infections. Some researchers have established that some nosocomial pathogens may survive on surfaces for months and therefore could be a continuous source of transmission if regular preventative surface disinfection is not performed20, it has also been established that fomites can be directly involved in the transmission of pathogens in health care environments21.
There have also been case reports of mycobacteria skin infections following body art tattooing which appear to be associated with dilution of tattoo pigments with non sterile fluids such as tap water 22, 23, 24, and also due to the use of poor quality tattoo pigments that were contaminated by multiple micro-organisms during manufacturing25, 33.
It has also been established by numerous studies that multi use consumable supplies can easily become contaminated by micro-organisms, the risk of contamination increases proportionally with the frequency of handling and the time frame from the point of original use/opening. For this reason single use, or lower frequency use and shorter time frames of use prior to disposal, are the best preventative choices. Key Points:
The Adequacy of Standard Procedures within the Salon-Clinic In practice it seems that sometimes use of the term “aseptic technique” does not actually reflect a Grade 2 Asepsis type procedural standard.
The General Salon Environment The general salon environment has the potential to harbour reservoirs of pathogenic micro-organisms on floors, walls, work surfaces, hand washing facilities, equipment, waste disposal receptacles and other objects that reside within that salon. Any inanimate object that has the potential to harbour micro-organisms and enable their transfer from person to person or from object to object is generally referred to as a fomite.
Sometimes fomites can be those objects that we can easily overlook, in 2011 the Department of Clinical Sciences and Administration, University of Houston College of Pharmacy, Houston, Texas USA published an interesting study evaluating the potential for an ordinary writing pen to become a fomite26.
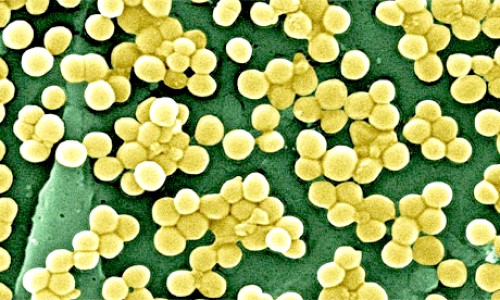
It was established that Staph Aureus demonstrated the ability to survive on a range of different pen types, with the longest survival time being 48 hours for pens with a rubber grip. The study concluded that pens may be potential fomites for health care associated pathogens. The risk of transmission by fomites, especially gram-positive cocci, was reduced by using alcohol-based sanitizing agents for wiping pens between attending patients26.
In addition to the obscure locations that can act as fomites the more obvious locations such as hand washing facilities can sometimes present risks that may be overlooked. In 2011 the Volta Regional Hospital of Ghana27 conducted broad scale swabbing of surfaces within the hospital in an attempt to identify those fomites that presented the greatest risk. The study had similar results to previous studies28 in that contaminated taps 25.8% tended to have the lowest total level of total bacterial colonisation but the most pathogenic isolates.
In other words taps tend to have fewer numbers of micro-organisms, most likely due to regular cleaning, but they also have the organisms that are most likely to cause infections. Perhaps one of the most interesting findings the study27 was that there was no significant difference in occurrence of total bacterial isolates before cleaning (87) and after cleaning (90) and some bacteria (Bacillus spp.) actually increased in number after cleaning was conducted.
What we can conclude from the above is that some micro-organisms will adapt and happily reside on the taps of hand washing facilities regardless of methodical cleaning practices. For this reason dedicated “hands free” operated taps reduce the risk of tap handles becoming a potential source of pathogenic contamination during a cosmetic tattoo procedure. You may be familiar with elbow operated taps often used in health care facilities however they have been shown not to be good choices in locations where lay staff are working because of the increased tendency for lay staff to operate elbow taps with their hands more frequently than might occur by health professionals.
In 2013 it was found that hand washing facilities in the intensive care unit of an Australian hospital was the most likely source of serious antibiotic resistant Hospital Acquired Infections due to bacteria growing in the sink traps31 and because of poor sink design it resulted in water splashing back from the sink onto the hands of health care staff during hand washing. The Division of Infectious Diseases, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA found that water saving electronically controlled taps emitted water that grew Legionella species more frequently than manual faucets36. It was believed that the additional faucet components may provide points of concentrated bacterial growth compared to more simplified systems.
Similarly it has been established liquid soap dispensers and hand sanitising liquid containers are also potential fomites29, 30, refillable soap dispensers that were contaminated with bacteria and disinfected prior to refilling returned to the same levels of bacteria within 7-14 days. It has been proposed that use of hands free operated dispensers may reduce the risk of contamination of hand sanitising dispensers.
Key Points: Regular cleaning and disinfecting procedures are an essential part of salon-clinic hygiene but alone they are not enough, careful selection of equipment for hand washing facilities are an essential part of the aseptic techniques within the salon. Recommendations would include;
Summary Undoubtedly the greatest risks of a client/patient developing a serious Salon Acquired Infection following Cosmetic Tattooing is if the tattoo service is provided by untrained technicians32, or if the technician is not complying with standard precautions and Grade 2 type aseptic techniques, or if un-sterile products and supplies are used33.
References
Date of most recent revision:
29/04/2013 (mutatis mutandis) Copyright © 2013 CTshop.com.au & the article author All Rights Reserved. No copying, transmission or reproduction of site content is permitted without our prior written consent.
Printing Restriction: This article is print disabled, please read our Intellectual Property & Copyright Policies if you would like to request a copy or permission to use the article content for any purpose. |
Main Menu
- Eyeliner Tattooing vs Dry Eye
- MicroBlading - First Things First
- Cosmetic Tattoo Training Standards
- Carcinomas in Tattoos a Statistical Anomaly
- Lash or Brow Growth Enhancing Serums & Tattooing
- What Influences the Colour of a Cosmetic Tattoo?
- Hygiene Protocols Update : Surface Cleaning Wipes
- Preventing & Managing Disputes
- Warm vs Cool Colours
- Age of The Alpha Metrosexual
- Who Will Buy a Poorly Iced Cake?
- Australia now has a Board Certified MicroPigmentation Instructor
- Robot Tattooists?
- Postcards From Birmingham
- The SCAPP Scale - Personalising the Micropigmentation Service
- How to Choose Your PMU Artist
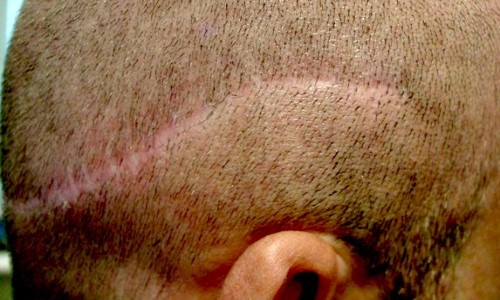
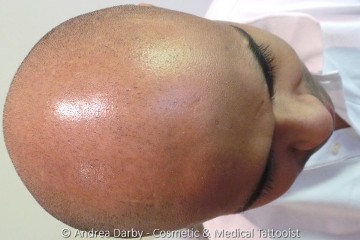
- Scalp MicroPigmentation - More Than Just Ugly Scars?
- Permanent Eyeliner - Avoiding Complications
- Personal Protective Equipment - Are You Covered?
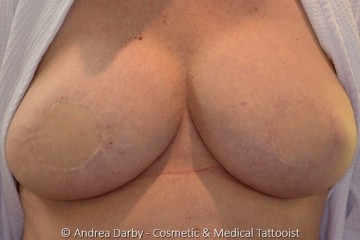
- 3D Nipple Tattooing a New Service?
- Why Do Cosmetic Tattoos Change Colour? - (Part 1)
- Why Do Cosmetic Tattoos Change Colour? - (Part 2)
- Smart Tattoos Are They The Future?
- Presentation: Adding Cosmetic Tattoo to Your Salon
- Cell Phone Vibrating Tattoos
- UK Survey - One Third Regret Their Body Art Tattoo
- Collaborating & Consulting with Dr. Linda Dixon
- Stem Cell Research - Inside the Lab
- When Marketing Via News Media Goes Wrong
- Client Pre-Treatment Screening Questionnaire
- Permanent Makeup Google Search Trends
- Potential Causes of Nosocomial Type Infections in the Salon-Clinic Setting
- Topical Anaesthetics & Cosmetic Procedures
- Introduction to the Fundamentals of Colour Perception
- Clients With Unexplained Loss of Outer Eyebrow Hair
- Hyperpigmentary Skin Conditions & Cosmetic Tattooing
- Cosmetic Tattooing & MRI’s - Diametric Particle Agitation Hypothesis (DPA)
Site News Selection
Educational Article Selection
Regulatory Article Selection
Client Case Studies Selection
Science Library Selection
Complete regrowth of hair following scalp tattooing in a patient with alopecia universalis
31/01/2023
Atypical Intraepidermal Melanocytic Proliferation Masked by a Tattoo: Implications for Tattoo Artist
20/09/2018
Chemical conjunctivitis and diffuse lamellar keratitis after removal of eyelash extensions
26/08/2018
Scarless Breast Reconstruction: Indications and Techniques for Optimizing Aesthetic Outcomes
07/04/2018
High speed ink aggregates are ejected from tattoos during Q‐switched Nd:YAG laser treatments
28/03/2018
Unveiling skin macrophage dynamics explains both tattoo persistence and strenuous removal
08/03/2018
Granulomatous Tattoo reaction with Associated Uveitis successfully treated with methotrexate
08/02/2018
Identification of organic pigments in tattoo inks & permanent make-up using laser mass spectrometry
07/02/2018
Microbiological survey of commercial tattoo and permanent makeup inks available in the United States
03/02/2018