Cart is empty
Topical Anaesthetics & Cosmetic Procedures
12/03/2013
by Derek Darby RN - Australian Registered Health Practitioner
Topical anaesthetics are sometimes used by service providers prior to minor cosmetic procedures that may otherwise cause the client/patient significant discomfort during the procedures. This document should be regarded as general information only and not a replacement for health or regulatory advice in any circumstances. This publication does not propose to encourage, advocate or promote the use of anaesthetics under any circumstances, always seek advice from a qualified medical practitioner and your local health regulator before using any form of topical anaesthetics.
▼ Continue Reading ▼
|
Important: This is not a how to guide it is a general discussion of the potential risks associated with the use of topical anaesthetics. The regulatory focus of this article is that which exists in Australia however the general principles can also be considered in other regulatory domains. I am happy to add to links that I have provided in Appendix 2 for regulatory information in other locations if they are both supplied and requested by others in different countries.
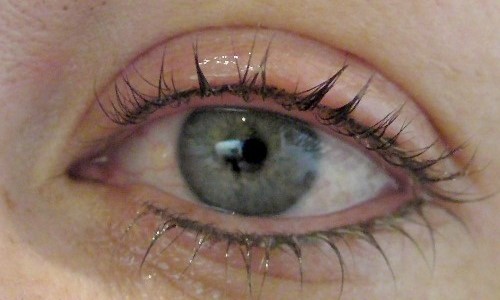
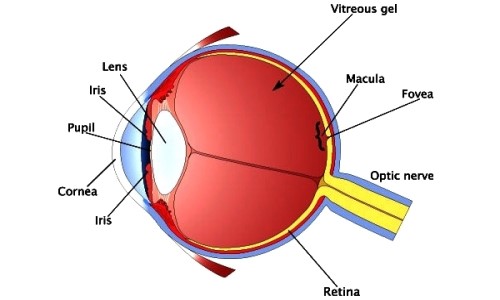
A pH scale which is most often described as a range between 0-14 is a logarithmic measurement of hydrogen ions H+ and the scale provides us the indication of acidity or alkalinity of a liquid, a pH of 1 having very toxic acidity (acid) and a pH 14 having very toxic alkalinity (caustic), distilled water is neutral with a pH around 7. Even if a topical anaesthetic is pH safe, if it is to be used on the face then great care should be taken to ensure the anaesthetic does not enter the eye because if the eye surface becomes anaesthetised then a corneal abrasion could easily occur inadvertently without the patient becoming aware, that is until the anaesthetic wears off!
Acquired methemoglobinemia is an uncommon though potentially life threatening blood disorder where an abnormal amount of the oxygen-carrying molecule haemoglobin builds up in the blood. In some of those cases the haemoglobin is unable to carry oxygen effectively to body tissues causing the patient severe hypoxic distress (low oxygen to the bodies cells). For the above reasons it is essential to ensure that topical anaesthetics are used sparingly and they are not applied to large areas of skin nor to areas where skin conditions exist, particularly if the surface of the skin is broken down. For example it would be contraindicated to apply a topical anaesthetic to an area of ulcerated, blistered or abraded skin as absorption may be much faster and the anaesthetic has a greater chance of entering the blood stream potentially affecting the client’s heart and brain as well as other internal organs. I cannot stress strongly enough the risks associated with misusing or overdosing a client/patient with a topical anaesthetic, if substances such as lidocaine enter the blood stream they can disrupt the normal; rate, rhythm, and co-ordination, of the hearts electrical system and its muscle function. Ultimately that could lead to significant slowing of the heart, dangerous hearth arrhythmias, seizures, cardiac arrest (the heart stopping altogether) and potentially death. Prior to purchasing and using anaesthetic products you should ensure that you are; 1) familiar with and in compliance of the Therapeutic Goods Act 1989 and the current Poisons Standard (see appendix 2). If in doubt contact the Therapeutic Goods Administration or if you provide services outside of Australia consult with your local health regulatory authorities.
Efficacy of Topical Anaesthetics Contrary to popular belief the concentrations of a topical anaesthetics active ingredients are not the sole factor in determining the efficacy of the product. There are several factors that will determine the efficacy of a topical anaesthetic product;
Caking/Heating Topical Anaesthetics You may have seen examples of topical anaesthetics being applied in a thick layer to the skin surface. I stress that caking of topical anaesthetics does not improve the efficiency of the product for anaesthetisation of the dermis, it does however substantially increase the risk of absorption of a dangerous amount of anaesthetic into the blood stream. It needs to be born in mind that the purpose of a topical anaesthetic is anaesthetisation of the dermis, which in most cases is only a fraction of a millimetre below the skin surface, you are not trying to cause penetration into the hypodermis/blood stream, so don't cake it on! You may have also seen examples of anaesthetics being warmed with external heating sources such as hot packs or plastic wraps or even ultrasonic stimulators. External heating and use of ultrasonic stimulators will cause blood vessels within the skin to dilate increasing transfer of anaesthetics into the blood stream.
Caution with Clients with low Body Weight & Both the Young & the Elderly You should be more cautious with the use of topical anaesthetics with clients/patients who have a low body weight this is because those with lower body weight will potentially develop a toxic blood serum level of anaesthetic quicker than clients with larger body weights, this is a due to the dose/Kg relationship. The young client/patient may also reach a toxic blood serum level quicker than an adult due to their smaller body mass and also due to metabolic differences that can be particularly potent with some ultra-rapid metabolizers. The elderly may also be at increased risk of potentially reaching a toxic blood serum level but for different reasons, as we age our heart rate tends to become naturally slower, we are more prone to hypo/hypertension and our hearts electrical conduction may become more susceptible to interruption by anaesthetics which can lead to the dangerous conditions of heart block, extreme bradycardia (slowing of the heart rate) or cardiac arrest. Also the liver and kidneys may be less efficient at breaking down and excreting anaesthetics meaning that lower doses may reach higher serum concentrations and have longer systemic duration than in the younger client/patient.
The Source of Topical Anaesthetics There are many places on the internet who are supplying topical anaesthetics such as tattoo equipment suppliers, 'quasi' medicine suppliers, cosmetics suppliers, permanent makeup suppliers etc. I will be blunt and state that I have no doubt that some of those sites are supplying anaesthetics illegally. Within Australia in most circumstances the only legal source of supply of a topical anaesthetic (in a percentage concentration that is at all likely to be effective) is a licensed pharmacist. Importing anaesthetics from overseas opens a whole new can or worms because you may potentially breach both the therapeutic goods act and customs regulations at the same time. Also many internet suppliers appear to offer little or no information about the concentrations of active ingredients within their product and virtially no information about the safe use of the product. If an client/patient had an adverse event involving the use of a topical anaesthetic that was obtained illegally it is highly likely that the service providers professional indemnity insurance would deny their insurance cover, in fact most policies have specific clauses denying liability if there have been any breaches of health regulations. For the above reasons in my view a service provider would be extremely foolhardy to obtain and use topical anaesthetics from any source other than from a licensed pharmacist and in full compliance with the applicable acts and regulations.
Appendix 1 Once again I stress this is not a how to guide it is merely a general discussion about some of the general safety precautions that should be considered by an appropriately qualified service provider before using any topical anaesthetic. The number one point here is that topical anaesthetics should only be used by persons who have been trained by a qualified health service provider and in circumstances that are in compliance with the law in your location.
02) Never apply anaesthetics on any woman who may be pregnant nor if they are breast feeding.
05) Never use any products containing epinephrine (adrenaline) near the eye, on fingers, toes, penis, earlobes, nose, nor inside the mouth. 10) Be extra cautious with the use of topical anaesthetics with clients/patients with low body weight e.g. below 55kg.
This list is by no means comprehensive however the client/patient should seek medical attention if any of the following side effects are experienced or observed after application of any form of anaesthetic products.
Links for Various Acts & Regulatory Authorities Australia Therapeutic Goods Administration Australian Capital Territory New South Wales Northern Territory Queensland Tasmania South Australia Victoria Western Australia
Date of most recent revision: 15/03/2013 (mutatis mutandis) Copyright © 2011-2013 CTshop.com.au & the article author All Rights Reserved. No copying, transmission or reproduction of site content is permitted without our prior written consent.
Printing Restriction: This article is print disabled, please read our Intellectual Property & Copyright Policies if you would like to request a copy or permission to use the article content for any purpose. |
||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Main Menu
- Eyeliner Tattooing vs Dry Eye
- MicroBlading - First Things First
- Cosmetic Tattoo Training Standards
- Carcinomas in Tattoos a Statistical Anomaly
- Lash or Brow Growth Enhancing Serums & Tattooing
- What Influences the Colour of a Cosmetic Tattoo?
- Hygiene Protocols Update : Surface Cleaning Wipes
- Preventing & Managing Disputes
- Warm vs Cool Colours
- Age of The Alpha Metrosexual
- Who Will Buy a Poorly Iced Cake?
- Australia now has a Board Certified MicroPigmentation Instructor
- Robot Tattooists?
- Postcards From Birmingham
- The SCAPP Scale - Personalising the Micropigmentation Service
- How to Choose Your PMU Artist
- Scalp MicroPigmentation - More Than Just Ugly Scars?
- Permanent Eyeliner - Avoiding Complications
- Personal Protective Equipment - Are You Covered?
- 3D Nipple Tattooing a New Service?
- Why Do Cosmetic Tattoos Change Colour? - (Part 1)
- Why Do Cosmetic Tattoos Change Colour? - (Part 2)
- Smart Tattoos Are They The Future?
- Presentation: Adding Cosmetic Tattoo to Your Salon
- Cell Phone Vibrating Tattoos
- UK Survey - One Third Regret Their Body Art Tattoo
- Collaborating & Consulting with Dr. Linda Dixon
- Stem Cell Research - Inside the Lab
- When Marketing Via News Media Goes Wrong
- Client Pre-Treatment Screening Questionnaire
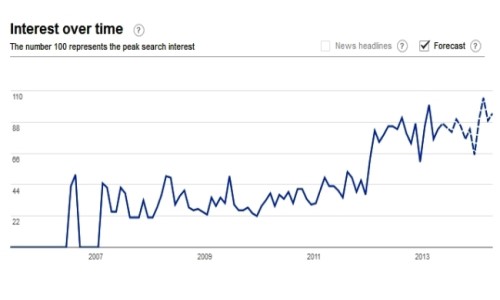
- Permanent Makeup Google Search Trends
- Potential Causes of Nosocomial Type Infections in the Salon-Clinic Setting
- Topical Anaesthetics & Cosmetic Procedures
- Introduction to the Fundamentals of Colour Perception
- Clients With Unexplained Loss of Outer Eyebrow Hair
- Hyperpigmentary Skin Conditions & Cosmetic Tattooing
- Cosmetic Tattooing & MRI’s - Diametric Particle Agitation Hypothesis (DPA)
Site News Selection
Educational Article Selection
Regulatory Article Selection
Client Case Studies Selection
Science Library Selection
Complete regrowth of hair following scalp tattooing in a patient with alopecia universalis
31/01/2023
Atypical Intraepidermal Melanocytic Proliferation Masked by a Tattoo: Implications for Tattoo Artist
20/09/2018
Chemical conjunctivitis and diffuse lamellar keratitis after removal of eyelash extensions
26/08/2018
Scarless Breast Reconstruction: Indications and Techniques for Optimizing Aesthetic Outcomes
07/04/2018
High speed ink aggregates are ejected from tattoos during Q‐switched Nd:YAG laser treatments
28/03/2018
Unveiling skin macrophage dynamics explains both tattoo persistence and strenuous removal
08/03/2018
Granulomatous Tattoo reaction with Associated Uveitis successfully treated with methotrexate
08/02/2018
Identification of organic pigments in tattoo inks & permanent make-up using laser mass spectrometry
07/02/2018
Microbiological survey of commercial tattoo and permanent makeup inks available in the United States
03/02/2018